Abdul Moiz Nadeem
Table of Contents
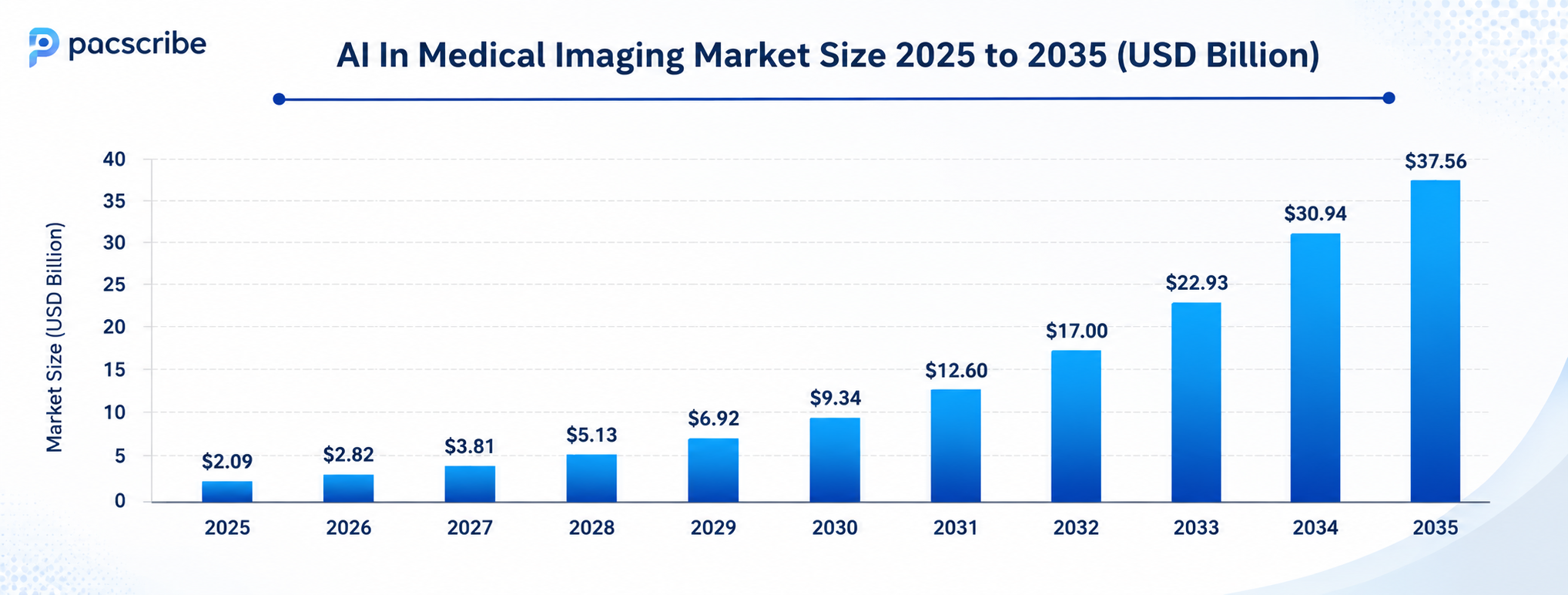
As radiology departments continue to handle higher imaging volumes, healthcare providers are increasingly adopting AI in medical imaging solutions to improve efficiency and reduce reporting delays. The global market was valued at around $2.09 billion in 2025 and is projected to grow rapidly in the coming years. From CT and MRI to X-ray, ultrasound, and mammography, these systems support radiologists with faster workflows and more consistent diagnostic reporting.
What is AI in Medical Imaging?
AI in medical imaging refers to the use of machine learning, deep learning, and neural network models to:
- Analyze medical images
- Detect anomalies
- Prioritize clinical worklists
- Support diagnostic decisions
- Generate preliminary structured reports
The models are trained on large imaging datasets, sometimes millions of annotated scans, to recognize patterns in pixel data that correlate with specific diseases, tissue states, or anatomical variations.
The software embedded within radiology systems that reviews scans as they come off the scanner, highlights findings worth a radiologist’s attention, and routes urgent cases to the top of the worklist. The radiologist still reads the scan and makes the clinical decision.
The AI provides a consistent analytical layer that does not fatigue, does not lose concentration on the 400th scan of a shift, and does not miss a finding because of time pressure.
AI systems are trained on large volumes of medical imaging data to identify patterns, anomalies, and disease indicators that may be difficult to detect through manual interpretation alone. This includes changes subtle enough to be invisible to the human eye at early disease stages.
Applications of AI in Medical Imaging
Cancer Detection and Oncology
- Oncology is where AI in medical imaging has produced the most clinically validated results, and the reason comes down to volume and stakes. According to the WHO, 1 in 5 individuals will develop cancer in their lifetime. Early detection is the single biggest determinant of survival outcomes.
- Mammography CAD systems historically raised radiologist sensitivity, and newer deep learning models often exceed those gains. In lung cancer screening, AI tools are now integrated into national programs.
- In February 2025, Coreline Soft launched in Australia specifically to support the National Lung Cancer Screening Program. GE HealthCare’s MyBreastAI suite, announced at RSNA 2024, streamlines radiologists’ workflows and offers advanced tools to identify and diagnose breast cancer at earlier stages.
- For routine chest CT scans, AI is being applied to analyze images for unexpected cardiovascular signals, flagging patients potentially at risk for heart disease by analyzing coronary anatomy, even when the scan was ordered for something else. This opportunistic detection is one of AI’s most distinctive capabilities.
Neurology and Brain Imaging
- AI is widely used for detecting brain tumors, assessing neurodegenerative diseases, and diagnosing conditions such as intracranial hemorrhage and stroke. For stroke patients, where treatment outcomes are measured in minutes, AI triage tools that flag critical CT findings and automatically alert care teams have direct survival implications.
- AI tools can also quantify brain changes like cortical thinning and abnormal protein buildup, associated with Alzheimer’s disease, supporting earlier and more confident diagnoses at stages when intervention is still meaningful.
- For multiple sclerosis, AI in medical imaging helps doctors track lesion plaques with precision: measuring their size, identifying new plaques, and detecting growth between serial imaging studies. These longitudinal tracking capabilities, applied consistently across every scan, are difficult to replicate with manual reading alone.
- NYU Langone’s research program at the Center for Advanced Imaging Innovation and Research (CAI2R) has trained deep learning algorithms to predict which patients with early osteoarthritis symptoms are likely to need total knee replacement, applying the same principle of predictive imaging to musculoskeletal medicine.
Cardiovascular Imaging
- AI applications in medical imaging for cardiology include automated measurement of cardiac function from echocardiography, identification of coronary artery disease from CT angiography, and detection of arrhythmias from cardiac MRI.
- HeartFlow’s FFR-CT analysis uses AI to model blood flow through coronary arteries from CT data, extending what imaging can tell clinicians beyond what the image itself shows.
- AI is also flagging incidental aortic aneurysms during imaging done for other purposes, routing those findings to vascular teams before they become emergencies. This kind of population-health benefit, where AI catches findings that were not the reason for the scan, represents a layer of safety that manual reading cannot consistently deliver under volume pressure.
Musculoskeletal and Orthopedic Imaging
- AI for fracture detection and classification is a growing area, particularly in emergency settings where X-rays are read under time pressure.
- Aidoc’s rib fracture triage tool, built on its CARE1 foundation model and cleared by the FDA, identifies fractures from CT to help prioritize patients who need urgent pain management or surgical evaluation.
- AI is also being applied to measure joint degeneration, track cartilage loss in osteoarthritis progression, and support pre-surgical planning in orthopedics. Specialized applications, including for sports medicine imaging, are extending AI into clinical environments outside traditional hospital radiology.
Radiology Scheduling and Reporting
- AI’s role in the radiology workflow extends well beyond reading the image itself. The full imaging chain contains multiple points where AI is now being deployed.
- AI can evaluate the appropriateness of an imaging referral based on the patient’s clinical history, providing guidance aligned with American College of Radiology (ACR) appropriateness criteria. This helps clinicians choose the right modality and ensures that scarce imaging resources go to patients who need them most.
- At the acquisition stage, AI is being embedded in scanner hardware itself, adjusting protocols in real time to optimize image quality for the specific patient. At the reporting stage, NLP tools can generate preliminary reports based on detected image findings, saving radiologists time and standardizing documentation.
- At KMC Manipal Hospital in India, AI-enabled CT workflows empowered clinicians to serve 20 to 30 more patients daily while maintaining diagnostic accuracy.
- AI-enabled triage systems have reduced average report turnaround times from 11.2 days to as low as 2.7 days, accelerating care delivery and allowing radiologists to dedicate more time to complex diagnostics.
AI in Medical Imaging: Market Trends
Benefits of AI in Medical Imaging
Diagnostic Accuracy
The clearest benefit of AI in healthcare medical imaging is reducing diagnostic error. AI models do not experience fatigue, distraction, or cognitive overload. Advanced algorithms can now process medical images such as chest X-rays, MRIs, and CT scans with unprecedented speed and accuracy.
Earlier Disease Detection
AI catches findings at stages when they are most treatable. Better image quality produced by AI reconstruction algorithms allows detection of the smallest traces of early cancer that conventional reconstruction might miss. Earlier detection directly affects survival rates and reduces the complexity and cost of downstream treatment.
Faster Scans With Improved Image Quality
AI tools now allow doctors to scan patients up to 75% faster, while also improving image quality, a development particularly important given that nearly one in three patients feels severe anxiety or claustrophobia in MRI scanners. Faster exams mean less patient discomfort and higher scanner throughput. Improved image quality means radiologists see more on every scan.
Radiation Dose Reduction
AI-based image reconstruction allows high-quality CT images to be produced from lower-dose acquisitions. Siemens Healthineers, GE HealthCare, and Philips have integrated deep learning reconstruction into their CT and MRI platforms, enabling diagnostic quality at radiation doses that would previously have produced unusable images. For pediatric patients and those requiring serial imaging, dose reduction is a meaningful clinical benefit.
Personalized Diagnostic Insights
AI can provide personalized insights based on a patient’s unique imaging data combined with other data points, electronic medical records, lab results, prior imaging history. This allows for tailored diagnostic assessments and treatment plans. It means clinicians can assess how a disease might be progressing for a specific patient, not just whether a finding matches a population-level pattern.
Addressing the Radiologist Shortage
The global radiologist workforce is not growing at the pace imaging demand requires. As of 2025, 54% of U.S. hospitals with over 100 beds report using AI in radiology, primarily for image interpretation (82%) and worklist prioritization (48%).
Generative AI in Medical Imaging
Generative AI in medical imaging is emerging as its own distinct application area. Where discriminative models classify what is in an image, generative models create or augment image data.
Image-centric work dominates, with GANs, diffusion models, and Vision-Language Models expanding limited datasets and accelerating diagnosis. Synthetic data generation is particularly important for rare conditions where annotated training data is scarce.
A model trained on 50 real cases of a rare tumor type will underperform one trained on 50 real cases augmented with 500 synthetically generated examples. This approach also addresses privacy constraints; synthetic images derived from real patient data contain no identifiable information.
In 2025, companies and research groups increasingly turned to advanced generative models capable of producing realistic, high-fidelity medical images without exposing patient-identifiable information. This privacy-preserving synthetic data approach is solving one of the biggest barriers to AI training in healthcare: patient data governance.
Challenges of AI for Medical Imaging
Data Quality and Generalizability
- It was found that chest X-ray models trained at a single institution showed up to a 20% drop in diagnostic performance when tested on external datasets. AI models can inadvertently learn site-specific characteristics, scanner calibration, imaging protocols, and patient demographics, rather than disease-specific patterns.
- Models trained on data from one hospital system may not perform at the same level at another. Diverse, representative training data is a prerequisite for generalizable AI.
Integration With Existing Systems
- AI tools need to connect with PACS for image data, RIS for radiology orders, and EHR systems for patient context. The digital images that radiologists read are produced in DICOM format and accessed via PACS.
- This means any AI tool deployed in a clinical workflow must be DICOM-compatible and integrate within that PACS environment. Without proper integration, AI produces outputs that clinicians cannot act on within their existing systems.
Longitudinal and Clinical Context
- Current AI systems often read each scan in isolation, without access to prior imaging or clinical history. A finding that is clearly pathological on one scan may be a known stable finding in a patient with a documented prior condition, a context that a radiologist brings automatically, but that AI must be explicitly given.
- Future AI architectures are addressing this through multimodal integration, but it remains a limitation in most deployed systems today.
Medical Devices and Artifacts
- Medical devices such as catheters, implants, prosthetics, and pacemakers significantly challenge AI algorithm performance, producing artifacts that can generate false positives or mask real findings.
- AI models need to be trained on datasets that include patients with these devices to perform reliably in general hospital populations.
Clinical Trust and Transparency
- While 85% of radiologists express optimism about AI in healthcare, only 59% of patients feel similarly confident.
- Referring physicians are more likely to trust AI when its outputs are transparent, legal responsibilities are clearly defined, and strong data protection measures are in place. Building that trust requires not just technical validation but a clinical communication strategy.
Regulatory Compliance
- FDA clearance for AI-based imaging tools requires demonstrated clinical validation, ongoing post-market surveillance, and defined change control processes.
- Algorithm updates can trigger new regulatory reviews. Organizations evaluating AI vendors should confirm FDA clearance status and understand what clinical validation data has been published, not just claimed.
The Future of AI in Medical Imaging
Several developments are shaping where AI in medical imaging diagnosis is heading over the next five years.
- Multimodal AI Integration: Models that combine imaging data with genomics, lab results, EHR history, clinical notes, and pathology data, producing integrated diagnostic support that answers not just “what does this image show” but “what does this image mean for this specific patient.” Research from CAI2R demonstrates this approach for early detection of cachexia in pancreatic cancer, combining CT images, clinical data, laboratory biomarkers, and LLM-extracted features from clinical notes.
- Autonomous Imaging Acquisition: In March 2025, NVIDIA and GE HealthCare announced a collaboration to advance autonomous diagnostic imaging through Physical AI, developing autonomous X-ray and ultrasound technologies using the NVIDIA Isaac for Healthcare platform. Fully autonomous systems that acquire, process, and flag imaging results with minimal manual technician involvement are moving from research into early deployment.
- Point-of-Care AI: AI embedded in portable and handheld ultrasound devices is making real-time AI-assisted imaging available in primary care, rural clinics, and low-resource environments. Siemens Healthineers’ December 2024 launch of the AI Abdomen feature in the Acuson Sequoia 3.5 ultrasound system, which automatically labels and measures organs in milliseconds, represents this direction.
- Predictive Imaging: AI models that estimate disease progression, identify patients at elevated risk based on imaging biomarkers, and determine when follow-up imaging is clinically indicated. These models shift AI from reactive (finding what is already there) to predictive (identifying what is likely to develop).
- Foundation Models at Scale: Aidoc’s CARE1 foundation model, Aidoc’s CEO, has stated the goal that by 2030, every complex diagnostic decision should be supported by AI that enables earlier detection and reduces preventable error. With $500 million raised and deployment at nearly 2,000 hospitals across 110 million analyzed cases, the infrastructure for that scale is being built now.
PACScribe By Folio3
Modern healthcare demands agility, and PACScribe by Folio3 is engineered to meet that challenge. As a cloud-native PACS medical imaging viewer, PACScribe eliminates the hardware constraints. It comes built in with Epic, ensuring seamless data flow directly into your EHR system. It has powerful AI-assisted report generation that reduces physician burnout and accelerates diagnostic turnaround times. Fully HIPAA-compliant and grounded in HL7 and FHIR standards, PACScribe represents the next generation of secure, interoperable medical imaging technology.
Closing Note
The tools are clinically validated, FDA clearances are accumulating rapidly, and hospital adoption is measurable. What separates organizations that extract real clinical value from those that don’t is implementation quality, specifically, how well AI tools integrate with existing PACS and EHR infrastructure, how clearly accountability between AI and clinician is defined, and whether the training data reflects the actual patient population being served. Health systems evaluating AI for radiology should look for vendors with documented validation studies and published clinical outcomes, not just compelling benchmark performance on controlled datasets. The model matters. The infrastructure around it matters just as much.
Frequently Asked Questions
What is the size of the AI in medical imaging market?
The AI in medical imaging market was valued at approximately $2.09 billion in 2025 and is projected to reach between $12 billion and $37 billion by 2034–2035, depending on the research source. Growth rates consistently fall between 25–35% CAGR, driven by rising imaging volume, chronic disease burden, radiologist shortages, and increasing regulatory support for AI-based medical devices.
How does AI improve medical imaging and diagnostics?
AI in medical imaging and diagnostics improves accuracy by providing a consistent analytical layer across every scan, one that does not fatigue, does not miss subtle findings due to time pressure, and does not vary by shift or radiologist experience level. AI tools flag urgent findings for immediate review, generate quantitative measurements that reduce interobserver variability, and produce preliminary report structures that reduce documentation time.
What is generative AI in medical imaging?
Generative AI in medical imaging is used to create synthetic imaging data for model training — particularly for rare diseases where real annotated examples are scarce. It is also applied to automated radiology report generation, where AI produces structured draft reports from image findings for radiologist review, and to image reconstruction, where generative models improve diagnostic quality from low-dose acquisitions.
What is radiomics, and how does AI enable it?
Radiomics is the process of converting medical images into large sets of quantitative features — shape, texture, intensity, spatial patterns, that can be analyzed by machine learning models to discover correlations with pathology, prognosis, and treatment response. AI makes radiomics clinically practical by automating feature extraction at scale, enabling the kind of population-level pattern recognition that would not be feasible through manual analysis.
What imaging modalities benefit most from AI today?
CT scanning currently holds the largest share of the AI in medical imaging market, at approximately 37%, followed by MRI and X-ray. CT dominates due to its widespread use in emergency, oncology, and vascular imaging. MRI AI is growing rapidly, particularly following advances like NYU and Meta’s fastMRI project that demonstrated 10x faster acquisition using deep learning reconstruction. Ultrasound AI is expanding significantly with portable and handheld devices.
What does the future of AI in medical imaging look like?
AI in medical imaging future trends include multimodal AI integrating imaging with genomics and EHR data, autonomous imaging acquisition systems, point-of-care AI on portable devices, predictive models that estimate disease progression rather than just current state, and explainable AI frameworks that give clinicians transparent reasoning behind flagged findings.
How does AI in medical imaging connect to broader healthcare IT integration?
It must connect to PACS for image data, RIS for radiology orders, and EHR systems for patient clinical context. Without these integrations, AI outputs exist outside the systems clinicians actually use. FHIR and HL7 standards provide the interoperability layer for these connections. DICOM compatibility is the baseline requirement for any AI tool operating on medical images.